A 40-year-old woman was seen six months after finding a swelling in her left breast. What was the course of treatment after the visit?
The diagnosis began with a breast examination
This woman, who is married and not menopausal, found a mass in the upper part of her left breast six months ago. The mass was hard to the touch, movable when pushed, and painless when pressed. The woman recalled that no other members of her family had malignant tumors.
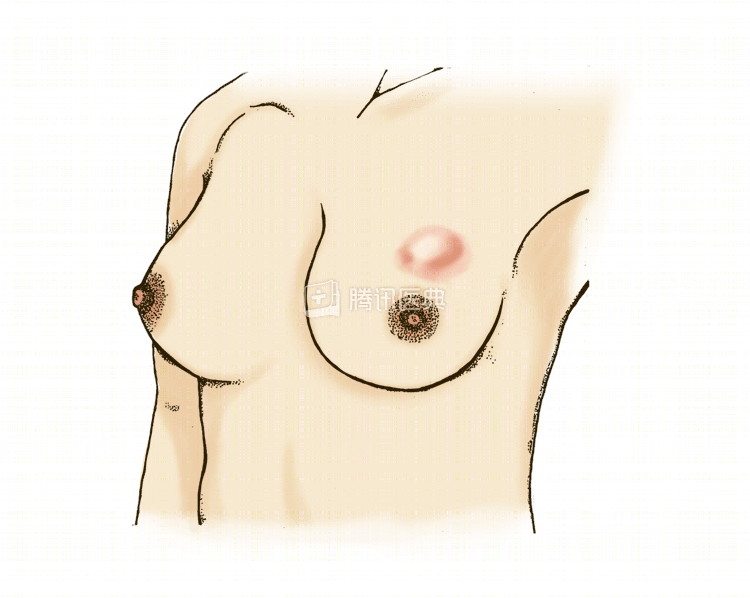
After questioning, the doctor performed a breast examination and found a 2.5-cm x 2-cm mass in the upper outer left breast that was tough and could be pushed, but the border was not clearly palpable. The doctor observed that the woman’s breasts were symmetrical, with no obvious depressions or uneven “orange peel-like changes” on the surface of the breasts, and no sunken, overflowing, cracked or ruptured nipples.
With these tests, the doctor initially suspected breast cancer and recommended imaging.
What are the suggestive effects of imaging?
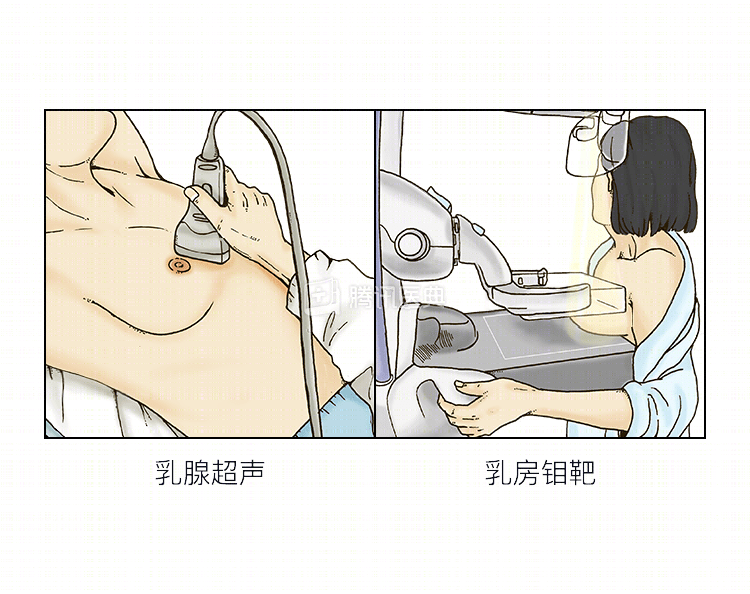
The mammogram (x-ray) reports a mass over the outer left breast and a Breast Imaging Reporting and Data System (BI-RADS) level 4C, suggesting further workup. The mammography report also suggested a hypoechoic mass in the left breast with a BI-RADS grade 4C.
What does the above report mean? In fact, whether it is an x-ray or ultrasound or magnetic resonance imaging (MRI), the conclusions of the report often appear with the abbreviation BI-RADS; just look at the number at the end. Overall, the smaller the number, the safer it is. The details are explained below:
- If the number is 0, the examination was not clearly seen or the observed image was incomplete and cannot be clearly assessed, requiring additional examinations;
- If the number is 1 and 2, no abnormality was found or the finding was a benign lesion;
- A number of 3 indicates a benign mass with a very low likelihood of being malignant, but requires careful follow-up;
- A number of 4 indicates that the likelihood of malignancy is increasing from 4A to 4C, which requires improved examination and is highly suspicious of malignancy at 4C;
- A number of 5 indicates that the tumor is a benign mass, which is very unlikely to be malignant.
- A number of 5 indicates a high probability of malignancy, but a puncture biopsy is still needed for clarification;
- A number of 6 indicates a high probability of malignancy.
- A number 6 indicates a definite diagnosis of cancer by biopsy before imaging is performed.
Pathologic diagnosis, key to confirming breast cancer diagnosis

The doctor recommended a puncture biopsy of the breast lump to clarify the diagnosis. The pathology report showed: invasive ductal carcinoma of the left breast, grade II, with no vascular aneurysm emboli. Immunohistochemistry showed: estrogen receptor (ER) (strongly positive, 90%), progesterone receptor (PR) (strongly positive, 80%), human epidermal growth factor receptor-2 (HER-2) (++), and cell proliferation index Ki-67 (30%+).
The histologic type and grading of the tumor are important elements of the pathology report. The pathologic findings of this woman showed invasive breast cancer, a common histologic type of breast cancer; with regard to grading, it is usually graded from I to III, reflecting the difference between the tumor and normal tissue, with higher grading indicating higher malignancy and grade II suggesting moderate malignancy. The ER, PR, HER2, Ki-67 and other indicators in the pathology report are immunohistochemical detection, which is an important basis for guiding treatment and can indicate which type of treatment the tumor is more sensitive to.
The doctor diagnosed the woman as having early-stage breast cancer with clinical stage IIA and molecular staging of Luminal B breast cancer based on immunohistochemistry. The 5-year survival rate for this type of early-stage breast cancer is 85% to 90% with standardized and appropriate treatment, which means that nearly 90% of patients survive for more than 5 years.
Patients can “decide” whether to have breast conservation
Treatment of early-stage breast cancer includes local treatment, mainly surgery, and systemic treatment, such as chemotherapy and endocrine therapy. In the case of similar treatment outcomes, the less damaging option, such as breast-conserving surgery + sentinel lymph node biopsy, can be chosen. This woman had early-stage breast cancer with a small tumor diameter, was expected to maintain good breast shape after breast-conserving surgery, and the axillary lymph nodes were not evaluated for metastasis, so her doctor recommended that breast-conserving surgery could be performed.
Many patients are concerned that breast-conserving surgery will not be “clean”. In fact, several large studies have shown that breast-conserving therapy combined with radiation therapy for early-stage breast cancer has similar survival and distant metastases compared to patients treated with total mastectomy. In addition, those who received breast-conserving treatment had a lower incidence of psychological disorders and were able to return to family and social life more quickly than those who had total mastectomy.
However, breast-conserving surgery is not “everything,” and requires postoperative radiation therapy as well as a range of adjuvant treatments and regular follow-up. Although breast-conserving surgery is essentially the same as the postoperative adjuvant treatment for total mastectomy, breast-conserving surgery needs to be combined with postoperative whole-breast radiotherapy, which can increase the cost and duration of radiotherapy-related treatment and, to a certain extent, the financial and psychological burden. Therefore, doctors will consider whether the patient is medically suitable for breast-conserving treatment, and patients need to fully consider their own economic conditions, medical conditions, and general health status before choosing breast-conserving treatment.
This woman declined breast-conserving surgery for financial reasons, so she underwent a total mastectomy + sentinel lymph node biopsy, which was a reasonable option for her.
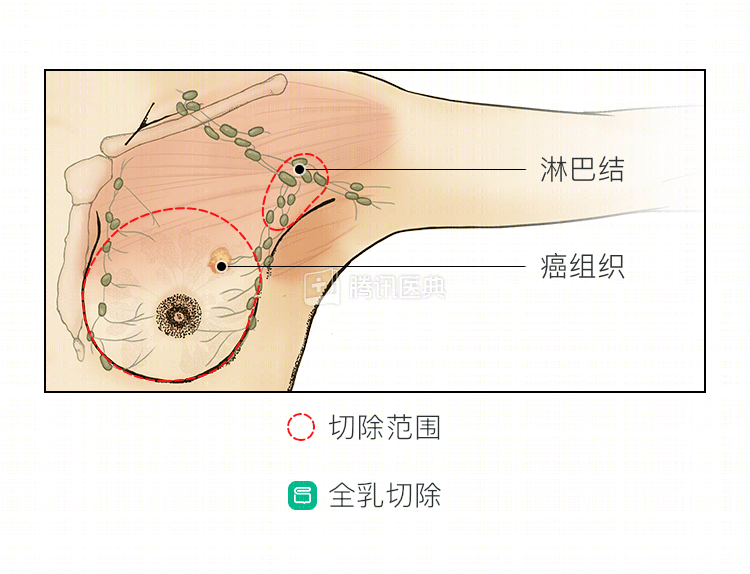
After a simple left mastectomy + sentinel lymph node biopsy, the postoperative pathology showed: invasive ductal carcinoma of the left breast, grade III, and no metastatic cancer in the sentinel lymph nodes. Immunohistochemistry report: ER (strongly positive, 90%), PR (moderately positive, 70%), HER2 (++), Ki-67 (40%+). On this basis, the woman was finally diagnosed as: left breast invasive ductal carcinoma pT2N0M0 stage IIA.
How was postoperative chemotherapy administered?
The goal of adjuvant chemotherapy for early-stage breast cancer is to strive for a cure, and it needs to be given in a standardized fashion, while the physician adjusts the dose or applies supportive therapy based on the occurrence of toxicities and side effects in chemotherapy, and individual variability.
The woman’s pathologic molecular staging was Luminal B breast cancer, histologic grade III, with a high grade suggesting high malignancy and a Ki-67 of 40%, consistent with the indication for adjuvant chemotherapy, and the examination showed good systemic status with no contraindications to chemotherapy. Therefore, the doctor recommended postoperative adjuvant chemotherapy. Considering other low risk factors for recurrence, including tumor diameter <3 cm, no lymph node metastasis, and high expression of ER and PR, AC regimen [Doxorubicin/Epirubicin+Cyclophosphamide] or TC regimen [Docetaxel+Cyclophosphamide] was recommended. Docetaxel)+Cyclophosphamide] for 4 sequential cycles.
Endocrine therapy, to do or not to do?
Postoperative adjuvant endocrine therapy is critical for patients with ER and PR-positive breast cancer. Because these hormone-receptor-positive breast cancers need to be nourished by estrogen for growth, blocking the nourishment of breast cancer cells by estrogen in the body with drugs can be a good way to inhibit the growth of cancer cells. Endocrine therapy has been proven to reduce the risk of recurrence and prolong the survival of hormone receptor positive breast cancer patients. It is now believed that endocrine therapy should be considered for patients with hormone receptor-positive breast cancer, regardless of their age, the presence of metastasis in lymph nodes, or the need for adjuvant chemotherapy. Endocrine therapy generally needs to be continued for 5 to 10 years to ensure complete killing of tumor cells.
Considering that the woman was not yet menopausal and had a relatively low risk of recurrence, the physician recommended oral tamoxifen (Tamoxifen, once daily) for 5 years at all ages, whether menopausal or not. After completing the standard 5-year endocrine therapy, if well tolerated, an extension of endocrine therapy to 10 years may be considered to further reduce the risk of recurrence, and a switch to another class of endocrine therapy, aromatase inhibitors, may be considered after menopause.
Doctors caution that regular follow-up visits should be made during endocrine therapy to monitor the condition and assess endometrial thickness, liver and kidney function, etc. If side effects or complications occur, the doctor should be seen and informed in a timely manner and will address them.
Summary: For early-stage breast cancer, breast-conserving surgery can be performed if the tumor diameter is small, the ratio of lesion to breast volume is appropriate, good breast shape is predicted to be maintained after breast-conserving surgery, and there are no contraindications to surgery, but the patient’s wishes are also an important factor in whether to perform breast-conserving surgery. The decision to perform and how to perform postoperative adjuvant therapy after breast cancer surgery is also based on the tumor condition and general health status.